No one really trains you on when a physician slips a report on the table and tells you that you have low sperm count. Majority of men sit there nodding, acting like they know it, then they go home and at midnight they type all that in the search engine. If that is where you are right now, this is written for you.
Oligospermia is not a rare disease. It impacts a massive population of men in most of whom had nothing wrong at all until they began to conceive a baby. People discuss the issue much less than they should, and it is important to note that this leaves the majority of men either ignorant or filled with unwarranted fear. Neither helps.
What is Oligospermia Meaning: Understanding the Basics
The word oligospermia (low sperm count) comes from the Greek. Oligo refers to a few or little. Spermia is sperm. They both characterize exactly what is occurring, less sperm than usual in the semen.
The benchmark that is set by doctors is 15 million sperm per millilitre. Go below that and you are in oligospermia land. That number may be big or small relative to your frame of reference, but the thing is not the number, in itself, it is what that number is in the context of fertility. A small number of sperm translates to less candidates traveling to the egg, and this decreases the chances of natural conception.
What is oligospermia, as well as this matter, is zero sperm. That is a separate condition called azoospermia. With oligospermia, sperm exists. They are just not showing up in the numbers needed to make things easy.
Doctors split the condition into mild, and moderate, along with severe based on how far the count has dropped. Mild is 10 to 15 million per ml. Moderate is 5 to 10 million. Severe is anything below 5 million. Naturally the lower it goes, the more attention it needs, but even severe oligospermia has treatment paths worth exploring.
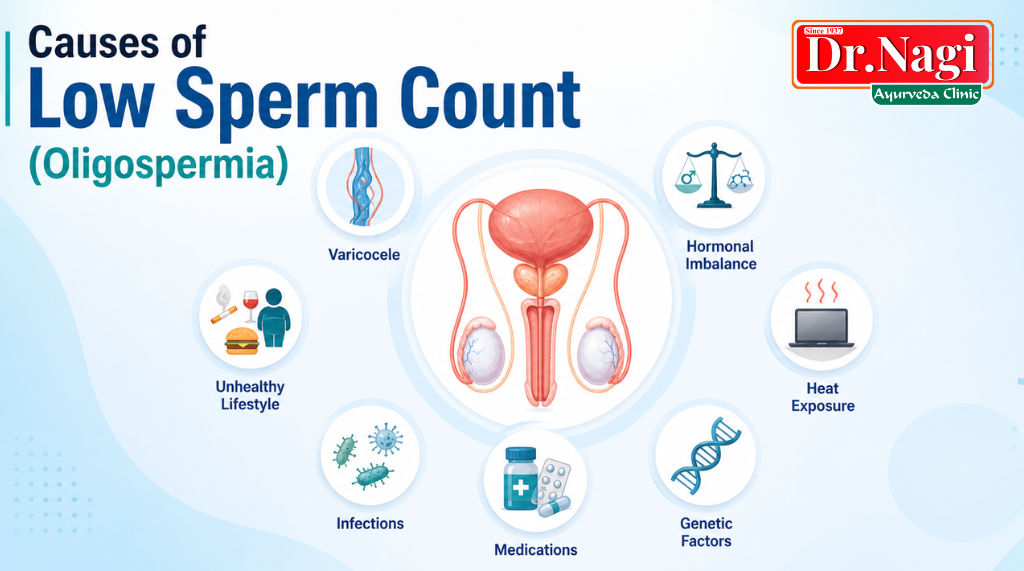
Oligospermia Causes: Why Low Sperm Count Happens
Low sperm count rarely has a single cause: it’s often a combination of male infertility, lifestyle, and environmental factors.
- Varicocele: Enlarged veins near the testicles raise local temperature, silently damaging sperm production over time
- Hormonal imbalances: Disrupted FSH, LH, testosterone, thyroid, or pituitary signals slow production significantly
- Lifestyle habits: Smoking, regular alcohol use, obesity, and chronic stress all negatively alter sperm quantity and quality
- Heat exposure: Prolonged sitting, tight underwear, and laptops on the lap cumulatively raise scrotal temperature
- Past infections: STIs like chlamydia and gonorrhoea can cause scarring or blockages; high fevers temporarily pause production
- Medications: Anabolic steroids, certain antidepressants, blood pressure drugs, and chemotherapy are notable culprits
- Genetic factors: Chromosomal conditions present from birth can affect reproductive development and function
A male infertility specialist evaluation helps identify which factors apply and what can be addressed.
Oligospermia Symptoms
This is genuinely the hardest part of explaining oligospermia to someone who has just been diagnosed. There are essentially no oligospermia symptoms that a man would notice on his own in day-to-day life.
No pain. No change in how sex feels. No physical difference in the ejaculate. No shift in energy, strength, or mood that would make someone think twice. A man can be training at the gym five days a week, eating well, sleeping fine, and still have a count well below what is needed for natural conception.
The most common low sperm count signs that actually brings men to a doctor is not any physical symptom at all. It is time, specifically, twelve months or more of trying to conceive without success. That is the moment most couples start investigating, and that is usually when oligospermia surfaces.
There are physical indicators that may at times lead to a problem. Pain or weightiness in one of the testicles especially when one has been in a long-standing standing posture can indicate varicocele. Testicles that have shrunk or become firm to the touch may be indicative of a hormonal or structural cause. Less development of body or facial hair, or a slow decline in sex drive may be an indication of a testosterone imbalance that may also be impairing the production of sperm.
These things on their own do not confirm anything. They are simply reasons not to delay getting a semen analysis done.
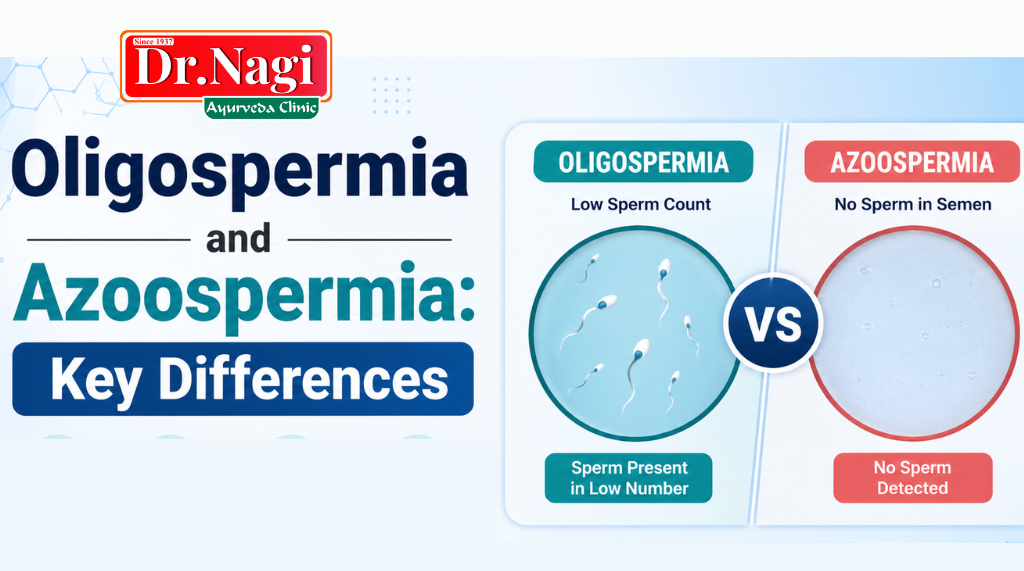
Oligospermia and Azoospermia: Key Differences
Due to the similarity between the two conditions in the sperm and the fact that both of them impair male fertility, they are confused frequently. However, oligospermia and azoospermia deal with different conditions that have different treatment implications.
Low and yet present sperm count. Azoospermia, no sperm in the ejaculate whatever. Azoospermia is either obstructive, where there is a physical barrier preventing the access of the semen to the semen despite the production of the same, or non-obstructive, where there is a failure in the production.
Oligospermia is generally the more treatable of the two. Not always easy, but more options exist and the outcomes tend to be better. Both require proper medical evaluation, guessing at treatment without diagnosis rarely goes well.
Oligospermia Treatment: What Are Your Options?
Treatment depends entirely on the root cause, diagnosis always comes first before any intervention is considered.
- Varicocelectomy: Varicocele correction is a minor operation that may be surgically corrected and recovered quickly; most men report an improvement in sperm count within three to six months.
- Hormonal therapy: Directional medication replenishes brain-to-testicle signalling, and thereafter sperm production positively responds.
- Infection treatment: Direct treatment of underlying infections allows the reproductive tract to recover naturally over time
- Lifestyle correction: Cessation of smoking, alcohol reduction, weight loss, stress management, and sleep repair can lead to actual, quantifiable changes in sperm count in months, in many men, this is the treatment.
- Ayurvedic herbs: Ashwagandha, Shilajit, Shatavari, Shivlingi, and Kapikacchu have centuries of recorded use in the support of male reproductive health, whose real mechanisms of action have not been fully elucidated, and are best used under the guidance of an expert.
- Assisted reproduction: At very low counts, IUI or IVF with ICSI provide possible avenues to conception with whatever sperm is available.
No single protocol fits all, the right approach is always tailored to the individual.

About Dr. Nagi Clinic
In Dr. Nagi Clinic, sexual health issues are addressed like any other health issue and Ayurvedic solutions are offered with confidence. Problems such as low confidence, early ejaculation, low stamina, phimosis and lack of desire can be corrected with proper counseling and attention. Since 1937, the focus has been on privacy, and safety, in addition to long-term Ayurvedic solutions, not quick fixes, but complete and lasting improvement.
The clinic is accessible across five locations:
- Ambala (Head Office): Sector 7, House No. 781, Ambala City. Every day, 9 AM to 7 PM. Other branches at Shop No. 128, Rai market, Near Gandhi ground, Ambala cant.
- Yamunanagar: Hotel Pooja, Near Fountain Chowk. Every Friday, 10 AM to 4 PM.
- Patiala: Near Old Bus Stand, Opposite Nehru Park. Every Thursday, 10 AM to 4 PM.
- Ludhiana: Kitchlu Nagar, Main Market, Arihant Tower, Near Punjab and Sindh Bank. Every Tuesday, 10 AM to 4 PM.
- Mandi Gobindgarh: Opposite Balu Ram Dharamshala, Near Punjab National Bank, Railway Road. Every Wednesday, 10 AM to 4 PM.
Contact: 9034772282 or 9416864455.
Products From Dr. Nagi Clinic
Pushkara Gold (₹2,000) – A classical formulation using supreme rejuvenating herbs and bhasmas from Ayurvedic tradition, known as rasayanas. Used by men to restore vigour and vitality, improve libido, reduce tension, and rebuild energy that has been gradually lost. Decades of trust behind this one.
Spermogen-120 (₹2,200) – Cold pressed 15 herbs: Shivlingi, Shatavari, Ashwagandha, Punarnava, Shilajit, Aloe Vera and Haritaki as tablets. Focuses on building reproductive system strength, sperm well-being, uterine mood, ovulation, and egg quality, in addition to implantation. Constructed with the purpose of helping couples to achieve natural pregnancy.
Chyawanprash (₹1,100) – A traditional Ayurvedic immunity and general wellness formula, part of the clinic’s broader health range.
Conclusion
Oligospermia may not show clear symptoms, but it can affect fertility if left unaddressed. The key is early diagnosis and understanding the underlying cause. With the right treatment, lifestyle changes, and medical guidance, many men can improve their sperm count and chances of conception. Seeking timely help can make a significant difference.
Frequently Asked Questions (FAQs)
Can my sperm count really be low without any signs?
Yes. Low sperm count produces no visible symptoms. Sperm production occurs silently within the testes, and a man can feel entirely healthy while having significantly reduced sperm levels. Only a semen analysis confirms it.
Will oligospermia always mean I cannot have children naturally?
Not necessarily. Mild to moderate oligospermia still allows natural conception, particularly when the underlying cause is addressed. Severe cases have assisted reproduction options available. A low count presents a challenge, not a definitive outcome.
How long before I can expect to see improvement from treatment?
It takes 74 days before sperm is completely developed. Any therapeutic, surgical, medical, or lifestyle-based, needs a minimum of three months before a follow-up semen analysis can indicate a significant, quantifiable change. Having patience is a biological requirement.
Does what I eat genuinely affect sperm count?
Yes. Zinc, selenium, and folate in addition to antioxidants are nutrients that support sperm production directly. Foods such as walnuts, eggs along with leafy greens are healthy. Further reduction in smoking, alcohol, and processed food also enhances better reproductive health outcomes.
Should my partner and I both get tested at the same time?
Yes. Concurrent testing is the most effective. A combination of male and female fertility tests give a complete view at an earlier stage without unnecessary time wastage whereby each partner is tested individually and at different times.


